Dying Twice: When Mourning Begins at Diagnosis
Can you really die twice and is it possible to live in between those deaths?
November is National Alzheimer’s Disease Awareness Month, first proclaimed as such by President Ronald Reagan in 1983.
Someone once told me that a person with Alzheimer’s disease dies twice.
It was a caregiver, who in an unguarded moment in front of a small group of communications professionals at a conference, that admitted to us that they felt like they lost their spouse once already when their spouse no longer recognized them or their children. They were preparing for the day when their spouse died and didn’t know how they would handle them dying a second time.
I thought about this on so many occasions during my year tenure as an Alzheimer’s Association employee. Our conferences would welcome people living in the early stages of the disease to take the stage and speak. They would tell their story and we would applaud them for their courage and bravery. They would be mini-celebrities for the rest of the week, as people took photos with them and their caregiver, paid extra attention to them, and just generally express our admiration for their fight.
We’d see them again the next year and they might be a little slower, but they were there and fighting the fight. And maybe the next year, or the year after that, their caregiver would come to the conference alone. They would tell us that their loved one wasn’t feeling up to the travel this year.
And then, some time after that, we would get the email from a colleague in that person’s home chapter delivering the inevitable news. Remember so-and-so from Advocacy Forum a few years ago…
The topic has swirled in my head since starting Dirt Nap, but emerged front of mind in something Brian Moritz wrote for his Griever’s Digest entry:
In the year after my mom died, I realized that I had been mourning her for a long time. She was so sick at the end. In a lot of ways, I feel like I lost my mom months before Kathy Moritz died. So I had grieved her loss long before she was gone.
In a lot of ways, this parallels with the topic of anticipatory grief. Pre-grieving a person’s death provides the forum to begin saying goodbye before a person dies, spreading those feelings out over a period of time rather than having it hit all at once.
There is a divergence for some. While I pre-grieved my mother’s death, I don’t feel like she died twice. Maybe she did for my sister, who was 15 or 16 and living at home from the time from her diagnosis to her death. Maybe she did for my father, who was there for the meetings with the doctors and who was involved in the decision making. I don’t know1.
So, I want to separate the ideas of dying twice from anticipatory grief and dive deeper into the former.
Twice?
I spent 18 years at the Alzheimer’s Association and knew a number of people who went from early stage to end stage. Every caregiver experiences something different because no two cases of Alzheimer’s (or other dementia) are the same, but there were the common threads:
The loss of independence. A working caregiver who found themselves in need of help because they eventually couldn’t leave their loved one home along during the day anymore. It’s often the first tangible sign that something is wrong or that the caregiver can’t handle it all on their own.
Memory decline. Let’s be honest, you can only laugh off someone repeating the same question over and over again for so long. Mix it with the stress of caregiving and it becomes annoying very easily. Giving yourself the grace of being frustrated is important, and as important as understanding that the disease is doing this, not the person. Admitting this, though, is admitting to the first death of Alzheimer’s.
(I learned about the validation method early on in my tenure. It’s more than just showing compassion for the person living with dementia; for the caregiver, it’s a new method of communication, using open questions, connecting emotion with emotion and opening a new door for the person with the disease to walk through. It doesn’t fix the memory issue, but it can help ease your own anxieties and concerns surrounding it.)The disconnection. I call my kids by the wrong names all of the time. That’s my wife and my fault for giving our kids names with hard L sounds. It’s the moment of looking into the person’s eyes and them not having any idea who you are, or so it has been told to me. No memory of you being their child or they your spouse. It’s as if they stepped into an alternate universe where you are just a friendly visitor.
The inability to function. The sense of smell degrades quickly for a person with a form of dementia. Speech, both in terms of selecting the appropriate word and the ability to talk, might erode. Movement becomes difficult, as motor skills degrade. Difficult behaviors may develop.
Yet, I heard the same thing about caregiving that I’ve heard about grief: that it was a gift. That they’ve never felt closer to the person they loved. It’s as if the anticipatory grief happened during the caregiving process.
But the mourning began at diagnosis.
Detour…
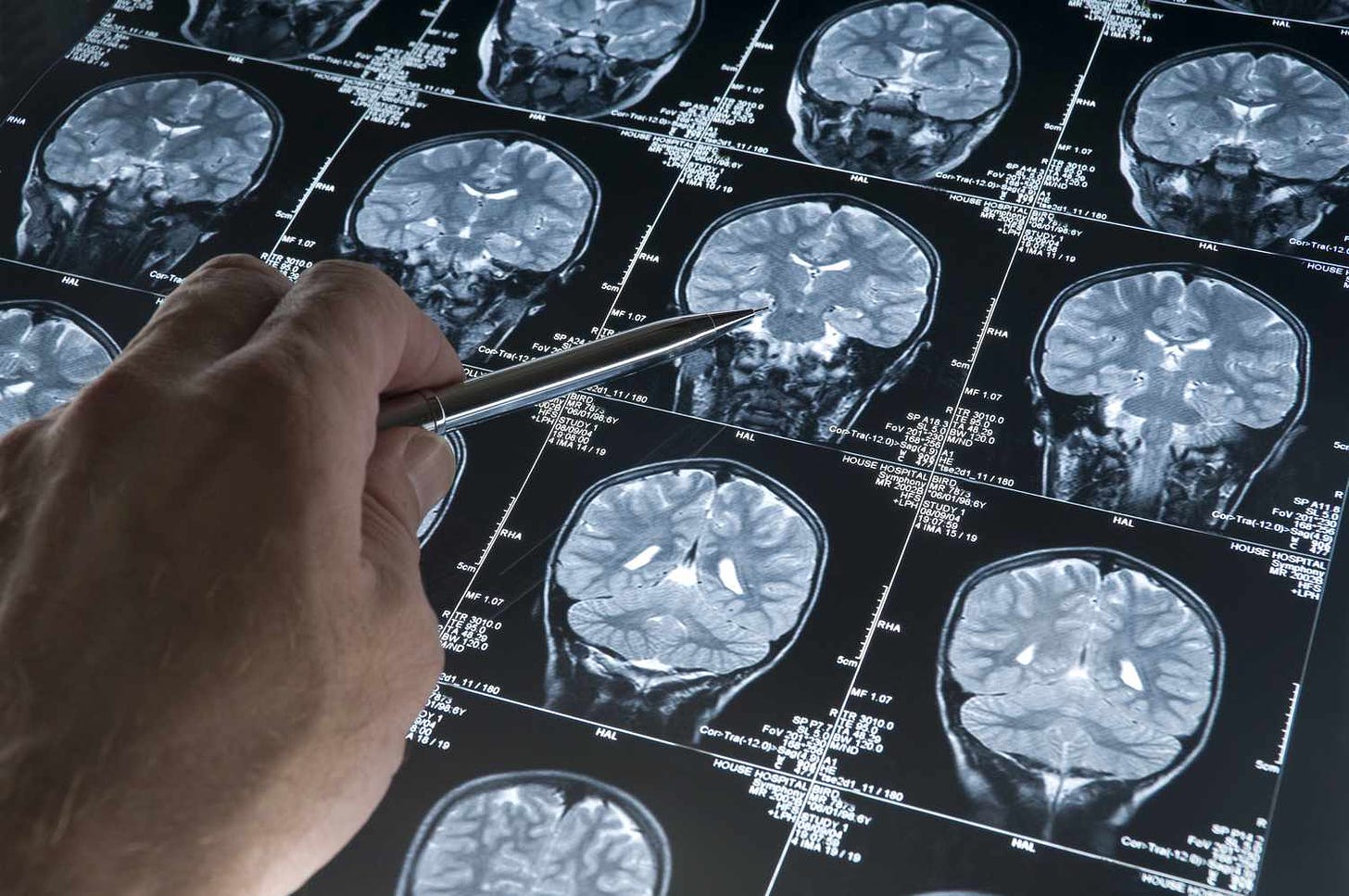
Dementia is a set of symptoms, including memory loss, issues with cognition, behaviors and other thinking abilities that interfere with daily life. Alzheimer’s disease, dementia with Lewy Bodies, Frontotemporal Dementia, etc. are the diseases under this umbrella. Each of them involve the brain deteriorating in different forms. None of them are curable, preventable or completely treatable, though leaps have been made on the latter. I’ll focus on Alzheimer’s here, since it’s the most common form of dementia.
Diagnosis is more than 90% accurate, if done correctly. Most general practitioners will just do a questionnaire and base their diagnosis on the score, but an accurate diagnosis of the disease requires a combination of tools — neuroimaging, cognitive testing and/or an exam by a specialist (geriatrician or neurologist). Christ, six in 10 healthcare professionals globally believe it’s a normal part of aging.
There’s no common path for someone living with the disease, but there are some shared threads about language, memory and movement. My grandmother lived more than 10 years with Alzheimer’s. I’ve seen others die three or four years after diagnosis. Your odds of developing Alzheimer’s increase with age — 1 in 3 over the age of 85 have it — but I’ve met people in their 40s with a definitive diagnosis.
Doctors, typically GPs, don’t always disclose the diagnosis. While the Alzheimer’s movement has brought the discussion to the forefront of society, it’s all to often whispered in the exam room. The GP doesn’t want to be the bad guy. The diagnosis should come from a specialist, but those are few and far between.
Getting old is awful. Just as youth is wasted on the young, aging is bullshit.
Finding purpose…
What caregivers of someone with Alzheimer’s may tell you was that the diagnosis hit like a truck full of bricks. It inspires the feeling of loss because everything is going to change and the immediate weight of the news triggers all sorts of emotions, guilt, abandonment and anger among them. Learning that someone you love has a terminal disease of any sort is that moment of the first death. The moment they draw the last breath is the second one. There is the question of who might die first: the person living with dementia or their caregiver. A study from the academic journal of the Alzheimer’s Association revealed that 18% of caregivers with dementia will die before the person they are caring for.
How you fill the moments in between are crucial. Going into mourning immediately does you no good; grieving is normal but mourning someone who is still alive is counterproductive. All of the major caregiving organizations offer the same advice — talk to someone, don’t ignore your feelings, don’t become isolated — because it’s the pathway to good caregiver health.
Finding purpose and community is something that I’ve watched people pursue with great success. Nonprofit disease organizations honor people living with their particular disease and will spend time teaching them how to use their voice for good. Maybe it’s as a speaker at a walkathon or education event. Maybe it’s as a volunteer. You know, it doesn’t work for everyone, but advocacy is a tool where someone with a terminal disease can find value. And it’s not trivial or token…it has real impact and you know it when you watch an elected official breakdown into tears after hearing from someone living with the disease (or their caregiver).
So, yeah, maybe it is possible for someone to die twice. But, it’s also possible to find fulfillment by living in between.
If you’re dealing with Alzheimer’s disease as a caregiver, child, sibling or friend, reach out to your local Alzheimer’s Association chapter. Their professionals are there to guide you through this journey.
Before memories became a memory…
If you’ve lost someone to Alzheimer’s or other form of dementia, I want to talk to you. I’d like to share your story with Dirt Nap readers as part of the Griever’s Digest. Reach out to me if you’re interested by emailing jaredpaventi at gmail dot com.
Final thoughts on finality…
Every man has two deaths, when he is buried in the ground and the last time someone says his name. In some ways men can be immortal.
— Ernest Hemingway
Dirt Nap is the Substack newsletter about death, grief and dying that is written and edited by Jared Paventi. It’s published every Friday morning.
We are always looking for contributors and story ideas. Drop us a line if you have interested in either space at jaredpaventi at gmail dot com.
I’m all over social media if you want to chat. Find me on Facebook, Twitter/X and Bluesky. I’m on Threads and Mastadon at @jaredpaventi, but I don’t check either regularly. You could message me on Instagram or LinkedIn, but I’m highly unlikely to respond.
Dirt Nap is free and we simply ask that you subscribe and/or share with others. The ego boost of inflated readership stats is all we need to get by.
I’ve never asked and I’m not sure it’s my business. This goes back to the singularity of grief and death. Everyone experiences a death differently.